UPDATE: The full transcript of the interview is now available. Here’s the relevant exchange:
BuzzFeed News: I want to move to the big LGBT news of yesterday, but first we had a very specific question from a reader who worked for you, a federal lawyer who’s transgender named Emily Prince. Federal policy bars discrimination against transgender people under health care plans covered under the ACA, but federal worker plans largely don’t cover gender reassignment surgery. Should they?
Obama: You know, I haven’t looked at that policy. My general view is that transgender persons, just like gays and lesbians, are deserving of equal treatment under the law. And that’s a basic principle. As you mentioned, my sense is that the Supreme Court is about to make a shift, one that I welcome, which is to recognize that — having hit a critical mass of states that have recognized same-sex marriage — it doesn’t make sense for us to now have this patchwork system and that it’s time to recognize that, under the equal protection clause of the United States, same-sex couples should have the same rights as anybody else.
I’m grateful that BuzzFeed asked the question, and I’m disappointed but not surprised by the President’s decision to pay lip-service to transgender equality and then move to “more comfortable” ground of marriage equality. The Administration has been dodging this question for approximately eight months now. Hopefully the OPM response to my Petition for Reconsideration will be more substantive.
BuzzFeed is interviewing President Obama on Tuesday and soliciting comments from their readership. Since they’ve been so solid on trans issues, I’m hoping this question that I submitted (or one like it) makes it through:
Mr. President, while the Justice Department is arguing that discrimination against transgender people is illegal, why does your Administration still choose to discriminate against transgender Federal employees in our health insurance?
95% of plans say they won’t cover anything related to being trans, and your Administration decided again just last June to let them do that. When will transgender Federal employees be able to choose these plans, confident that our care will be covered?
Follow-up:
You said in the State of the Union you wanted to advocate for transgender people on the world stage. How can the U.S. be a credible voice on these issues while continuing to directly discriminate against trans people in employment, in military service, in health care?
In June 2014, the Office of Personnel Management announced it would “remove the requirement” for transition-related care to be excluded from health insurance coverage. This left the exclusion at the whim of insurance companies. Ever since, I have been pressing the Office of Personnel Management quite hard to ask – why were insurance companies permitted to continue discriminating against transgender Federal employees?
In July 2014, I held a meeting with the White House Office of Information and Regulatory Affairs to ask that question. They had no answer then. When the rule was published I submitted a Petition for Reconsideration, formally asking OPM to reconsider its decision to not address this ongoing discrimination on the basis of gender identity within the Federal government. I demanded the records that OPM held concerning the choices plans were making as to covering or not covering transition-related care. I continued to press OPM for answers during a November 2014 town hall with Federal employees, and they continued to have none. The records request was finally handled, with only a brief period between the response and the end of Federal open season, when Federal employees became locked into their health plans for another year.
In December 2014, associated with the Department of Labor rulemaking regarding Federal contractors, I sent a letter to OPM (alongside DOL) asking about this continued discrimination against transgender Federal employees. That letter has yet to receive a response.
Just two weeks ago, during a civil rights symposium at my employing agency, I sent OPM a question about trans-exclusionary health insurance for their open question-and-answer session on employment topics. OPM declined to respond, stating that a response would be provided in writing at a future date.
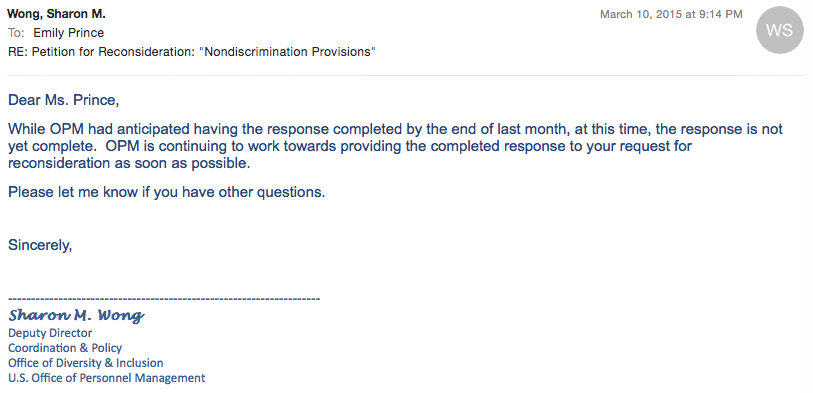
To date, OPM has yet to respond to my August 2014 Petition for Reconsideration, though they have suggested a response will be forthcoming this month. To date, OPM has not responded to my many questions circling around this key point:
Why were insurance companies allowed to continue to discriminate against transgender Federal employees by excluding coverage for transition-related care?
When will it stop?